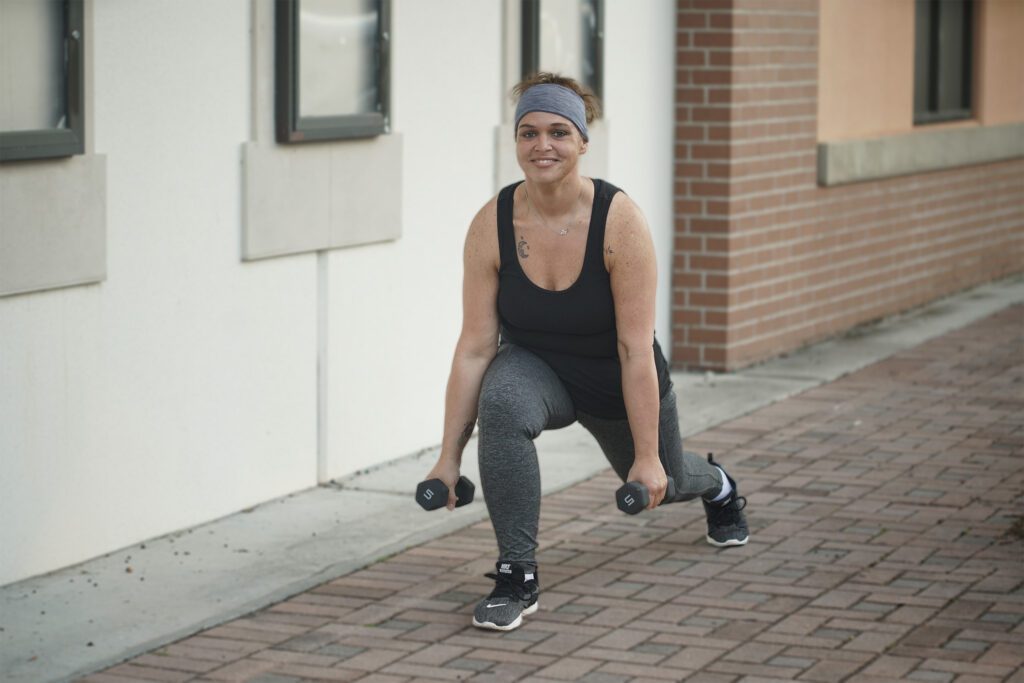Winter Haven Operating Room Technician Opens Up About Her Weight Loss Surgery and Journey
by TERESA SCHIFFER
photos by APRIL SPAULDING
Elizabeth Lawhorne was living a life of frustration and poor health before she made a decision that would change her life forever. Lawhorne was 356 pounds with serious health issues, including high blood pressure, sleep apnea, and prediabetes, plus a family history of heart disease, when she began researching bariatric surgery as an option. In particular, she was interested in gastric sleeve surgery, a bariatric procedure that removes 75-80% of the stomach. It is now the most commonly performed bariatric procedure in United States and worldwide.
“In the beginning of 2018, I decided that having gastric sleeve surgery was probably the best thing that I could do,” the Winter Haven operating room technician says.
“I had tried diet and exercise on my own and it didn’t work out very well. I had PCOS (polycystic ovary syndrome) pretty bad, and it doesn’t make it very easy to lose weight.” Lawhorne recalls.
Lawhorne learned of bariatric surgeon Dr. Clinton Hall through some co-workers who had undergone sleeve gastrectomy surgery. Hall is a board-certified surgeon with BayCare in Winter Haven. He has assisted hundreds of patients in their successful surgical weight loss journeys. The patient’s weight loss odyssey does not begin and end with a surgical procedure, however. There is a process of preparation and aftercare involved that will ultimately transform the patient’s lifestyle.
The process begins with an informative video, after which the patient chooses a surgeon. Lawhorne had heard good things about Hall, who has been practicing surgery for a decade after completing his fellowship in surgical weight loss surgery at Ohio State University. Once the decision to move forward was made, Lawhorne had four sessions with a dietician, followed by a meeting with a psychiatrist and then a fitness instructor. The entire process took about six months.
Once the surgery was scheduled, Lawhorne was given a two-week diet to adhere to. She describes the surgeon’s instructions to her prior to surgery, “Dr. Hall told me that if I didn’t do my two-week diet like I was supposed to, he would know, and if my liver hadn’t shrunk enough to do the surgery he would close me up and he wouldn’t do it.”
The pre-surgery diet consists of a high-protein, liquid regimen comprised of four protein shakes per day, plus a list of other approved foods with water or milk. Lawhorne needed to eat six times daily, so between protein shakes she could have sugar-free Jell-O, plain oatmeal, Dannon Light & Fit or Greek vanilla yogurt, celery, tomatoes, carrots, onions, broccoli, cauliflower, or unsweetened applesauce.
“The first week it’s hard – very hard,” Lawhorne describes of the special diet. “But once you get past the first week, it gets easier.”
Lawhorne followed the diet faithfully, despite being tired of the protein shakes after a week, and her sleeve gastrectomy was performed on August 29, 2018. This was Lawhorne’s first surgery, so she had some apprehensions about going under the knife, but she trusted Hall and took his advice to get up and walk as much as possible after the procedure. Within a week she found herself pain-free and walking on a daily basis.
After the surgery, Lawhorne was on a liquid diet for the first 11 days. The next 14 days was a pureed food diet, for which she simply bought baby food, as it was the easiest way to ensure she was consuming a nutritious, high-protein diet. Lawhorne was limited to 4-ounce servings at each meal, with a restriction on drinking anything for 30 minutes after eating. After the 14 days of pureed food, Lawhorne was able to move on to eating soft foods, such as mashed potatoes, chopped hamburger meat, chicken breast, and some vegetables, but always in 4-ounce meals, and being sure to eat the protein first, in case she got full and couldn’t finish the full 4-ounce allotment.
Hall lauded Lawhorne’s efforts at her one-month and three-month followup appointments, and she was cleared to take up activity at a gym in order to help facilitate her weight loss. The surgeon’s goal was to help Lawhorne decrease her weight to under 200 pounds. At the time, she didn’t take him seriously. Despite her doubts, she resolved to reach a target weight of 180 pounds.
At her one-year check-in with Hall, Lawhorne weighed 182 pounds. “I was mad at myself for those little two pounds!” Lawhorne chuckles, but the support staff at BayCare’s bariatric unit was enthusiastic about her outstanding progress, and she continued to maintain the lifestyle changes she had made, such as exercising regularly and eating better.
Now, a little more than two years years after her surgery, Lawhorne is proud to report that she now weighs 165 pounds — putting the total weight lost at 190 pounds. She has since moved from walking to running several times a week, and continues to monitor what foods she eats in order to minimize carbohydrates and get plenty of protein. Success stories like Lawhorne’s are what makes Hall proud to be in this line of work.
After undergoing bariatric surgery with him, Hall tells his patients that they have joined a weight loss “family.” He and his team take great joy in seeing the major improvements that his patients make in their health and lifestyles, and always likes to see a patient experience a complete resolution of their obesity-related illnesses.
Hall sums up the benefits of bariatric surgery nicely, “Seeing their smile, the new smaller clothes that they have purchased, and noting their significantly shrinking medication lists are some of the best rewards as a weight loss surgeon. I’d like readers to understand that choosing bariatric surgery means embracing a new, healthier lifestyle in all aspects and requires effort from the patient, as Elizabeth’s story shows. Weight loss surgery is a “tool” to be used to achieve the goal of both increased quantity and quality of life and is highly effective when used the correct way.”